By Daniel Dunaief
The flu season has hit with a vengeance in February, as a seasonal virus that can be deadly has become the dominant cause of illness in the area.
Suffolk County hospitals reported 337 residents with influenza in the week ending Feb. 1, according to New York State Department of Health data.

Just last year, for the 2023-2024 flu season, Suffolk County hospitalizations peaked on Dec. 30 at 52. Even in the year before, when people were starting to wear masks much less frequently than during the peak covid years, flu hospitalizations in the county peaked at 50 on Dec. 17.
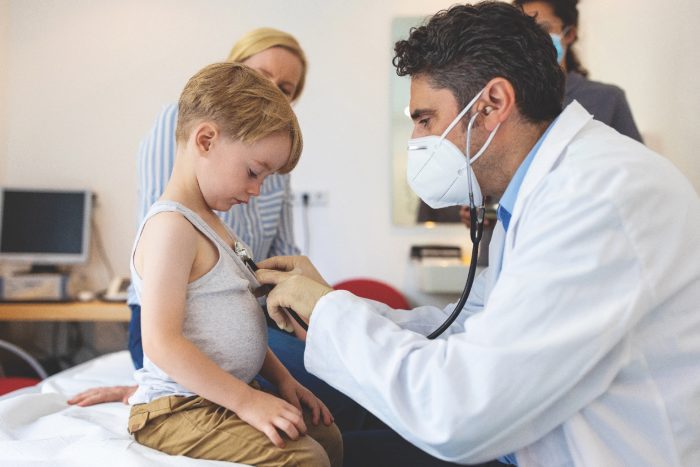
“We are definitely seeing more people sick” with flu, said Dr. Sharon Nachman, chief of the Division of Pediatric Infectious Diseases at Stony Brook Children’s Hospital. The emergency room is “wildly full, and even urgent care walk in is full.”
The number of positive cases of flu A at Stony Brook University Hospital in January was 800. That compares with 400 cases for the same strain last year, according to Nachman.
While the flu is cyclical and can cause different levels of infections from year to year, local doctors suggested that the overall flu vaccination rate was lower this year, which may have increased vulnerability to the virus and extended the time people exhibited symptoms.
The number of people vaccinated is “incredibly lower compared to past years,” said Nachman. On top of that, people may not have been exposed to the flu for several years amid measures to reduce the spread of Covid-19.
Residents’ immune systems may have “no good memory response” if the last exposure to the virus occurred some time before 2020, Dr. Nachman added.
The dominant strain of the flu this year is the A strain, which accounts for about 80 percent of the cases.
Nachman suggested that people who were vaccinated in early September may not have as much resistance to the flu this month, as their peak resistance, which typically lasts about three months, has wained.
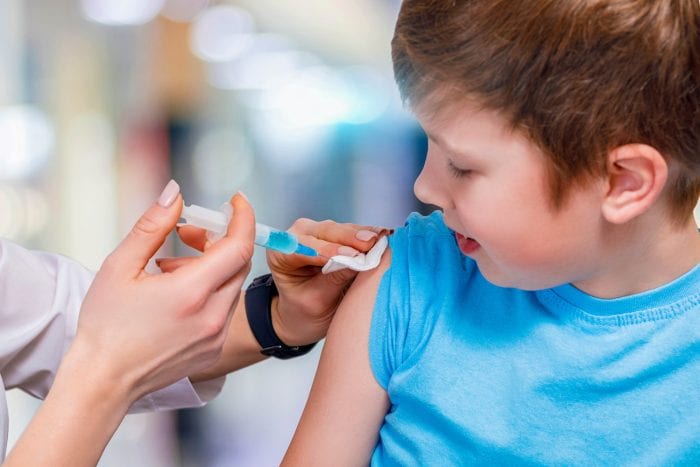
Health care professionals added that people who haven’t been vaccinated could still receive the shot, as the flu season could continue to last for a month or more.

“It is not too late to get the flu shot,” Dr. Gregson Pigott, Commissioner of the Suffolk County Department of Health Services, explained in an email.
Dr. Adrian Popp, chair of Infection Control at Huntington Hospital, said the staff has been offering flu shots for residents who have were not already immunized.
“I don’t know how much longer this will last,” said Popp. “It’s still cold and it’ll be cold in March.”
Typically, it takes two weeks for the body to receive full protection from the shot. The shot does provide some incremental benefit immediately.
“You start building immunity from the moment you get” the shot, said Popp.
So far this year, there have been two deaths at Huntington Hospital, which is not unusual for the flu.
Mortality from the flu is “turning into what it used to be,” said Popp, with deaths at about pre pandemic levels.
High risk patients
High risk patients are typically older or have preexisting conditions.
People who have an inability to fight infections can get “much sicker from the flu,” said Dr. Alan Bulbin, St. Francis Hospital and Heart Center Director of Infectious Disease.

Health care workers urged those who are in higher risk groups either to see their doctors if they start developing symptoms or to use some of the at home tests, including a recent one that can test for flu A and B, as well as Covid.
“If you are immunocompromised, you should have a low threshold,” said Bulbin. “You should speak with a doctor, go to urgent care, and do a swab. That may differentiate influenza” from other infections such as respiratory syncytial virus, or RSV, and Covid.
The antiviral treatment Tamiflu can be effective if people start taking it within 48 hours of developing symptoms. Paxlovid, meanwhile, can also help within a few days of developing covid.
“We urge residents, especially those at risk for severe illness, to contact their medical providers at the onset of symptoms,” Pigott explained in an email.
Lower Covid and RSV levels
While the flu has infected a larger number of people than in previous years, the incidence of RSV and Covid has declined.
In Suffolk County, 90 residents are hospitalized with Covid, while the number of deaths from the virus is 29 since the start of the year, according to the New York State Department of Health.
That compares with 190 residents hospitalized last year and 96 deaths from Covid from Jan. 1 through Feb. 14.
“The virus that causes Covid-19 is still circulating and causing disease, although not as aggressively as in previous years,” Pigott explained.
RSV, meanwhile, rose in the fall, peaked in late December and has been falling since then.
RSV accounted for 0.2 percent of emergency department visits on Feb. 1, Pigott added.
Future ID doctors
Specialists in infectious disease were unsure how the pandemic affected the interest among doctors in training and residents in their field.
For some, the appeal of reacting to fluid circumstances and to gathering insights about a developing disease that could and did affect billions of lives could be appealing. For others, however, the demands, the hours, and increasing politicization of medicine as well as the divided response to vaccines could have pushed them in other directions.
“Am I concerned that not enough people are going into the specialty?” Nachman asked. “Yes.”