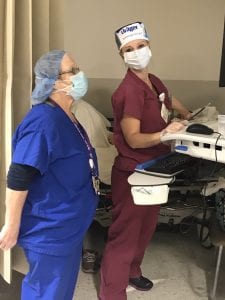
St. Charles Hospital ICU nurse Kacey McIntee, walking through the halls of a hospital in the midst of a pandemic, is just one of scores of RNs who have watched their world flip the wrong way around.
Where once the hospital had one Intensive Care Unit, now it has three. Every time she gets to work, she slips into hospital-issued scrubs and she’s assigned to one of the three units. Every single bed is housing a patient on a ventilator, nearly 40 in all. She’s bedecked in a mask, hair covering and face shield.

Typically, the ratio is two ICU patients to one ICU nurse. However, now there are cases where she cares for up to three patients, alongside a helper nurse. She starts her day by looking at her assigned patients’ charts, and then spends the rest of her 12-hour shift doing her best to keep these patients, many in such dire straits, alive.
“A lot of times you can kind of expect something is going to go bad just based on blood values alone,” she said. “We mentally prepare ourselves for the worst-case scenario with our patients.”
It’s a common story among many medical centers, but local hospitals St. Catherine of Siena Medical Center in Smithtown and Port Jefferson’s St. Charles, both in the Catholic Health Services system, have been on the front lines of fighting the virus for longer than others, having seen their first COVID-19 positive patients March 8.
Jacquelina VandenAkker, a 33-year veteran respiratory therapist at St. Charles and Port Jeff resident, said while the past week has shown what seems to be a plateauing in the number of new cases, the first 10 days of the virus “was hell. You didn’t know the end of it.”
“We felt it was literally such a war zone. You knew you could be a victim to it because you don’t understand it,” she said.
Hospital officials confirmed there were a number of staff who have contracted COVID-19, but declined to release the number of employees who have been infected, citing that staff did not want it known if they’ve been previously infected.
“We see a lot of deaths,” the respiratory therapist said. “I take the same unit. I know my patients. We start to understand the disease a lot more.”
McIntee, a Sound Beach resident, knows the pain and suffering of the COVID-19 patients suffering. It’s hard not to become entangled in the lives of these people, knowing the pain of suffering when the family can only communicate via tablet computer and online video chats.
“Nurses are really, really good at coping mechanisms,” she said. “One of the most useful ones is humor and the other is detachment. We cannot picture our loved ones in the bed — if we hear that one of our loved ones is sick with COVID, all bets are off, we are a mess.”
When it comes to that, when what has universally been the once inconceivable is happening moment to moment, McIntee said they rely on their fellow nurses.
“It’s almost as if we’re all in war together, and we have this bond for life that we will always be connected together, that we had these experiences that really nobody else in the world can experience except during this time,” she said.
The Initial Wave and Beyond
Jim O’Connor, the president of St. Charles and chief administrative officer of St. Catherine of Siena, said hospitals faced initial difficulties but hope things continue to look up.
“Both St. Charles and St. Catherine had their first COVID-19 patient on the same day,” he said. “We struggled to keep up with it and the personal protective equipment we needed in that first week. Thankfully we seem to have gotten our sea legs.”

Only about 25 percent of patients who are diagnosed require hospitalization, but of that 25 percent, 50 percent require ICU care, and many of them require a ventilator, O’Connor said.
Even before Gov. Andrew Cuomo’s (D) mandates shutting down all essential businesses, hospital admin said they saw what they call a “surge” of patients.
Bonnie Morales, the director of infection prevention for St. Catherine, said she and other specialists at hospitals around Long Island had started preparing for the “what ifs” a few weeks before it finally came, but even then, it was hard to estimate just how much it would overtake the entire health care system.
“I would have to say we were prepared, but that line list [of staff procedures] I went back to in the beginning, has grown from a page to three pages long,” she said.
The precautions for reducing infections became one of the most supreme considerations with both patients and staff, she said. Morales, a Selden resident, said the average patient on “transmission-based precautions” which were before only meant to help patients and staff avoid contact, has now gone from 20 to 30, up to over 100 that are currently on these transmission-based precautions because of the virus.
The hospitals had what the admin called a surge plan, but as the St. Charles president put it, “a man plans, and God laughs.” Learning just how many beds they would have to increase to was staggering, but he thanked the admin team who worked with barely little notice to start the process of acquiring more beds and space.
After Cuomo announced an executive order mandating hospitals increase their bed capacity by at least 50 percent, St. Charles and St. Catherine have boosted the number of beds to 243 in St. Charles and 296 beds at St. Catherine.
Mike Silverman, the COO at St. Catherine, said early on the hospitals decided to close access to the public. It was something that was unpopular to start, but in hindsight has been a smart decision.
Silverman only joined the hospital little more than two months ago and has had a trial by fire in the truest sense of the phrase.
“I don’t think anybody thought this was going to happen,” he said. “There was no playbook for this … It’s a lot of people doing what needs to be done,” he said.
O’Connor said the hospitals hit a high in the number of patients in the previous weeks, but since they have been climbing, inch by strenuous inch, off of that peak. Since the start of the outbreak, St. Charles has gone from eight ventilators to nearly 37 at peak. St. Catherine had 35 at peak. Each hospital has transformed its space to accommodate the massive number of critical patients by creating two new ICUs in each. All elective surgeries have been suspended and those workers have been moved to aid COVID-19 patients.
“There’s definitely some angst,” Silverman said. “We know how many people are dying in the state, and we would see this many deaths in a week. It’s tough, whether it’s at work, whether its friends or friends’ families.”
Both admin and health staff agreed the community has done an incredible amount of support for the health care workers. There have been consistent donations of meals, snacks and drinks. There have been a rollout of homemade masks and PPE supplies as well, along with cards and notes thanking the health care workers for all they do.
Still, to say it hasn’t taken an emotional toll would be wrong.
“It has been very tough on the staff because there is a very high mortality rate for people on ventilators,” O’Connor said. “What compounds it we weren’t allowed to have visitors so that really adds a whole different isolation for the patient and the families.”
The hospital has been using tablet computers to connect patients with family members at home, but it has also meant having to give them difficult news about those family members remotely.
“They have their own fears understandably about it. They have their own families they go home to that they worry about spreading it to,” he said. “I give them so much credit for them to put themselves at risk to be in a room with someone with a contagious disease.”
There have been moments of hope throughout the day in between the darkness. Every time a patient comes off a ventilator, the hospital plays “Breathe” by Faith Hill over the loudspeaker. When a patient is dismissed from the hospital, they then play the classic Beatles song “Here Comes the Sun.”
Hospitals’ PPE
O’Connor said the hospitals sterilize the PPE used by hospital workers at the end of each shift, and after the N95 is used three times then it is discarded, though if it becomes “soiled or contaminated” then it is discarded before that. Normally, such masks are not designed to be reused, but with supplies tight, hospitals and other medical centers have been looking to get as much use out of equipment as possible.

“We know it is not a perfect system,” O’Connor said. “Nobody expected to have this patient volume, but I think we’ve done a good job, but is it perfect? No.”
The federal Office of Emergency Management has added to supplies, along with donations from companies and other local individuals. The U.S. Centers for Disease Control has made guidelines for decontaminating such equipment, and hospital administration said they are following those guidelines. Catholic health systems announced earlier this month they had created an ultraviolet light sterilization system for masks in CHS hospitals.
The New York State Nurses Association has taken issue with the hospital’s practice of reusing such PPE as N95 masks after they’ve been sterilized. The union points to mask manufacturer 3M, who said there were no disinfection methods that would kill the virus and maintain effectiveness, though the CDC’s website cites numerous sources related to the positive results of disinfecting such masks.
Though a union representative could not be reached by press time, nurse representatives have spoken to other news outlets saying that both hospitals lacked PPE supplies, and that unlike systems, nurses in St. Charles and St. Catherine were made to wear gowns for an entire shift that are meant to be disposed of after one patient encounter.
McIntee said at the start of the pandemic, things were confused with PPE, with the CDC changing its guidelines constantly. Regarding gowns, she said hospital workers have a choice, they can either spray down reusable gowns with a cleaning solution in between patients, use disposable blue/plastic gowns, or the so-called bunny suits, the full-body white suits with a hood. With face shields, there are no other choices than rinsing it with solution.
Now, McIntee said if a worker wears an N95 mask continuously throughout the day in a 12-hour shift, they can discard them. If they wear them intermittently throughout the day, then they are bagged and sent to be sterilized at night. Sterilized masks then can be worn intermittently three more days before they are discarded.
“Not once have I ever had an issue with the N95 masks being told ‘no, you can’t have one,’” she said. “I’ve always been able to have access to any PPE I wanted … Now I think we have a system down, and it’s less anxiety.”
St. Catherine April 22 accepted a donation of gowns and masks from the Kings Park Chamber of Commerce, and Morales said the bevy of donations they have received have truly helped in the fight against COVID-19. The hospital has received donations of tie back and bunny suits.
Regarding St. Catherine staff reusing gowns, Morales said “We are giving out supplies for the staff to utilize and they have what they need in order to take care of their patients.”
O’Connor said the hospitals have been doing multiple things to aid the front line workers, including bringing in agency staff and repurposing staff from outpatient to inpatient services to add more hands on deck. The hospitals have developed quiet rooms for staff to catch their breath, and Silverman said St. Catherine has a service where staff can purchase basic items, they have little time to get from working long days during the pandemic.
“It would be very foolish for us to not keep our staff safe,” O’Connor said. “Why would we possibly not be doing anything we can to keep them safe?”







