By Leah S. Dunaief

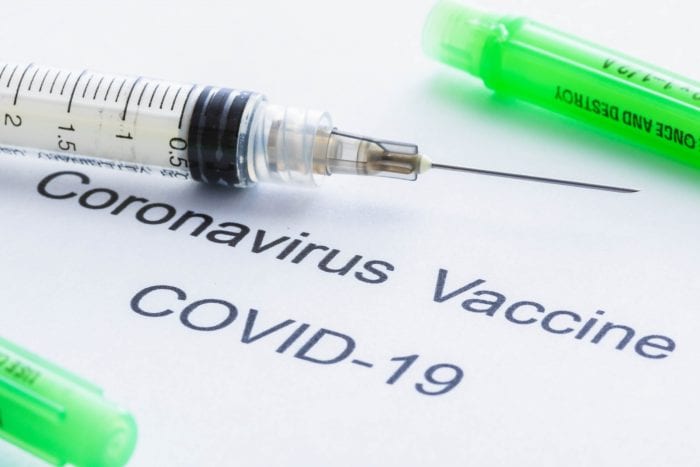
The days of 2020 are running down now, with only half of December still remaining, but the BIG news stories certainly aren’t letting up. Just this past Monday, two historic events were reported. One was the first vaccinations in the United States against the novel coronavirus. The other was the ratification by the Electoral College of the vote for our next president. Both were climaxes to enormous efforts, but they were not ends in themselves.
Many people will continue to be angry with the election result and keep protesting. And many will still become ill and some will even die before universal vaccination, victims of the worst pandemic since the flu of 1918.
We watched both memorable occurrences happening in real time on television this week, and we know they are turning points for us in the new year. Probably like you, I have had enough of the political scene, but I would like to dwell on getting tested for the virus until we are able to be vaccinated, perhaps a matter of some months. There is a lot of fresh and interesting information to share. The following comes from The New York Times:
There are four reasons to get tested. The most obvious one is if you feel sick. Symptoms of the virus include fever, dry cough, fatigue, headache or loss of smell and taste. Many tests are most reliable during the first week of symptoms.

Another reason is if you think you may have been exposed to an infected person or if you were in a risky situation like an indoor gathering or on an airplane. If so, quarantine and get tested five or six days after the possible exposure to give the virus a chance to be detectable. Quarantining should be for at least seven days.
Some people are tested simply as a precaution, especially if you are going for dental work or another medical procedure. Colleges and boarding schools test students before they leave campus and again when they return. They have largely had good outcomes following this procedure. And finally, some people will choose to be tested if there is a high level of infection in the community.
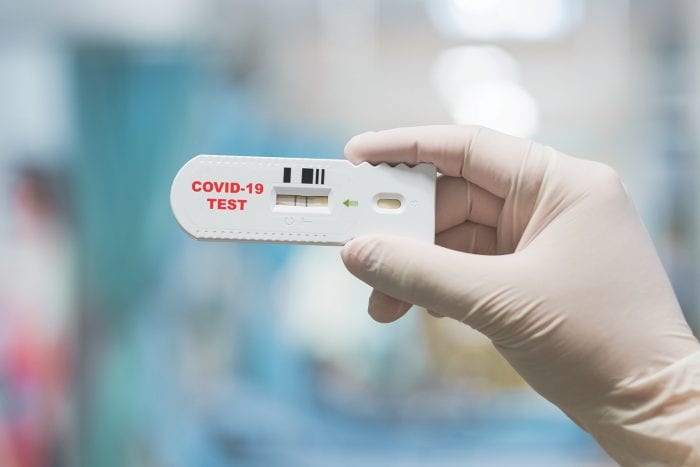
There are different types of tests, but they all use a sample from the nose, throat or mouth. Most widely used is the PCR test that looks for pieces of the virus’ genetic material. This is the most accurate but takes the longest — three to ten days — for the results to come back from the lab.
The antigen test detects coronavirus proteins and is among the cheapest and speediest with results in about 15-30 minutes. This is recommended as often as several times a week, since the results, both negative and positive, are less accurate. In one study, this rapid test missed 20 percent of the infections.
Then there is the rapid molecular test, which combines the reliability of molecular testing with the speedy results of an antigen test. Abbott’s ID Now and Cepheid Xpert Xpress use portable devices that process the sample right in front of you. This test is highly sensitive and can detect the virus a day sooner than the antigen, but it is not quite as reliable as the lab test, and while rapid, may take a little longer. Again a negative result is not foolproof, and you should continue to wear a mask and practice social distancing.
If you test positive, you should stay home and isolate. Tell others you have been with so that they may get tested. You should wait 10 days after symptoms started and 24 hours after a fever ends before going out. If results are negative, you might still be infected. Test again. False negatives happen.
Home testing kits are starting to be available, and Dr. Anthony Fauci likes the idea. New Jersey is one state that is offering them. Results are delivered in a day or two after being sent in, and one company that has received the FDA green light for at-home testing is Lucira.
There are walk-in testing sites in the area, although they usually have long lines. Appointments can be made on Stony Brook University campus by calling 888-364-3065.