News Flash: Generated by ChatGPT, edited by our staff
• FDA approves RSV vaccines for the first time. These vaccines target the respiratory syncytial virus, a seasonal lung-related illness, with recommendations for adults over 60 and pregnant women in specific gestational weeks.
• Infants under eight months born to mothers without the RSV vaccination can receive monoclonal antibody treatment, providing immunological protection against severe RSV symptoms.
• There are challenges in accessing RSV shots, including delayed processing by insurance companies and pharmacy shortages. Health officials urge residents to advocate for themselves, emphasizing the importance of timely vaccinations given the approaching RSV season.
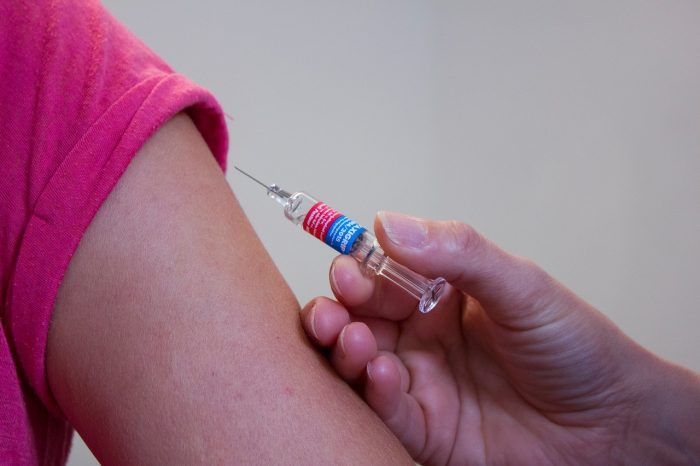
For the first time, vaccines against the respiratory syncytial virus, or RSV — a lung-related illness that crops up during the fall and winter — have been approved by the U.S. Food and Drug Administration.
The FDA recommends that adults ages 60 and older receive a dose of the vaccine, either Pfizer’s Abrysvo or GSK’s Arexvy, within the next few weeks.
Women in their 32nd to 36th week of pregnancy at some point during September through January are also urged to receive Abrysvo.
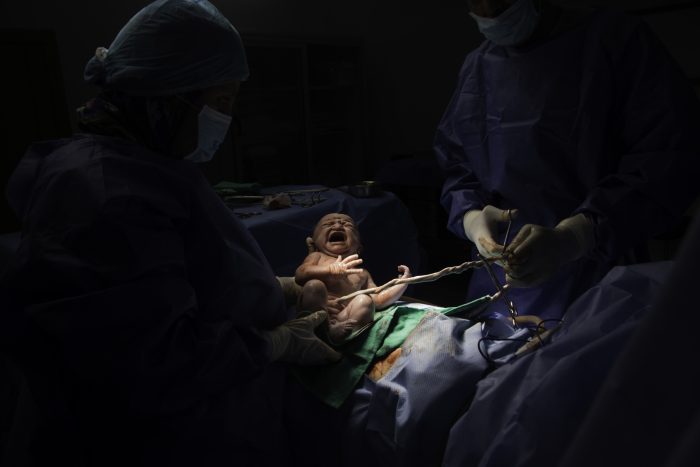
For babies born to mothers who didn’t receive a dose of the RSV vaccine, the FDA has approved a monoclonal antibody treatment for infants eight months old and younger that will offer immunological protection against a common and prevalent respiratory condition that can lead to severe symptoms and hospitalizations.
Additionally, the Centers for Disease Control and Prevention recommend a dose of RSV antibody for children between eight and 19 months entering their second RSV season if they have chronic lung disease, are severely immunocompromised, have a severe form of cystic fibrosis or are American Indian or Alaska Natives.

While local doctors welcomed the opportunity to inoculate residents, they said finding these treatments has been difficult.
“People are having a hard time getting” the vaccine, said Dr. Sharon Nachman, chief of the Division of Pediatric Infectious Diseases at Stony Brook Children’s Hospital.
Some pharmacies have told patients to come back, which decreases the likelihood that they will return for vaccinations in time, Nachman said.
Additionally, insurance companies have not immediately processed requests for vaccinations, which also slows the process, she said.
Nachman recommended that residents “continue to go back and advocate for yourself” because that is “the only way you’ll get what you need.”
RSV season starts around November, which means residents qualified to receive the vaccine or parents with infants need to reach out to their health care providers now to receive some protection against the virus.
Childhood illness
According to recent data, RSV caused 2,800 hospitalizations per 100,000 children in the first year of life, Nachman said. The range can go as low as 1,500 per 100,000.
However, that only captures the number of hospitalized people and doesn’t include all the times anxious parents bring their sick children to doctor’s offices or walk-in clinics.
“Hospitalizations are the worst of the group, [but] it’s a much bigger pyramid” of people who develop RSV illnesses, Nachman said.
In addition to recommending monoclonal treatment for children under eight months old, the CDC urges parents to get this treatment for vulnerable children who are under two years old.

Like other vaccinations, the RSV vaccine won’t prevent people from getting sick. It will, however, likely reduce the symptoms and duration of the illness.
“In trials, RSV vaccines significantly reduced lower respiratory tract lung infections serious enough to require medical care,” Dr. Gregson Pigott, Suffolk County Health Commissioner, explained in an email.
At its worst, the symptoms of RSV — such as fever, cough and serious respiratory illness — are problematic enough that it’s worth putting out extra effort to receive some immune protection.
“If you’re a little kid or an elderly patient, this is a disease you don’t want to get,” Nachman said.
Pigott said that data analysis shows that RSV vaccines are 85% effective against severe symptoms of the virus.
While people can receive the COVID-19 and flu vaccines simultaneously, doctors recommend getting the RSV vaccine two weeks later.
According to preliminary data, eligible residents may benefit from the RSV vaccine for two seasons, which means they would likely need to receive the shot every other year, according to Pigott.
With two vaccines approved for adults, Pigott recommended that people receive whichever shot is available.
“Both reduce a person’s chances of getting very serious lung infections,” Pigott explained, adding that several measures can help people protect themselves from the flu, RSV and COVID.
Getting a vaccine, washing hands, avoiding touching your eyes, nose or mouth, avoiding close contact with people who are sick with respiratory symptoms and wearing a mask in places where respiratory viruses are circulating can all help.
Those who are symptomatic should stay home when they are sick and wear masks when they are around other people.
Suffolk County Department of Health Services officials indicated they are aware of the challenges of getting shots and monoclonal antibodies and “ask people to be patient.”