By David Dunaief, M.D.

Despite the best efforts of public campaigns and individual physicians, heart disease is still the number one cause of death in the U.S. (1). To put that in perspective, every 33 seconds, one person dies of heart disease.
While some risk factors are obvious, others are not. Obvious ones include family history, high cholesterol, high blood pressure, obesity, sedentary lifestyle, diabetes and smoking. In addition, age plays a role in risk: men at least 45 years old and women at least 55 years old are at greater risk. Less obvious risks include gout, atrial fibrillation and osteoarthritis.
The good news is that we have more control than we think. Most of these risks can be significantly reduced with lifestyle modifications.
How much role does weight really play in heart disease risk?
Obesity continually gets play in discussions of disease risk. But how important is it, really?
In the Copenhagen General Population Study, results showed an increased heart attack risk in those who were overweight and in those who were obese – with or without metabolic syndrome, which includes a trifecta of high blood pressure, high cholesterol and high sugar levels (2). “Obese” was defined as a body mass index (BMI) over 30 kg/m², while “overweight” included those with a BMI over 25 kg/m².
Heart attack risk increased in direct proportion to weight. Specifically, there was a 26 percent increase in heart attack risk for those who were overweight and an 88 percent increase in risk for those who were obese without metabolic syndrome.
It is true that those with metabolic syndrome and obesity together had the highest risk. However, it is quite surprising that obesity, by itself, can increase heart attack risk when a person is “metabolically healthy.” Because this was an observational trial, the results represent an association between obesity and heart disease. Basically, it’s telling us that there may not be such a thing as a “metabolically healthy” obese patient. If you are obese, this is one of many reasons that it’s critical to lose weight.
Do activity levels really affect heart disease risk?
Let’s consider another lifestyle factor; activity levels. An observational study found that these had a surprisingly high impact on women’s heart disease risk (3). Of four key factors — weight, blood pressure, smoking and physical inactivity — age was the determinant as to which one had the most negative effect. Those under the age of 30 saw smoking as most negatively impactful. For those over the age of 30, lack of exercise became the most dominant risk factor for heart disease, including heart attacks.
For women over age 70, the study found that increasing physical activity may have a greater positive impact than addressing high blood pressure, losing weight, or even quitting smoking. However, since high blood pressure was self-reported, it may have been underestimated as a risk factor. Nonetheless, the researchers indicated that women should make sure they exercise on a regular basis to most significantly reduce heart disease risk.
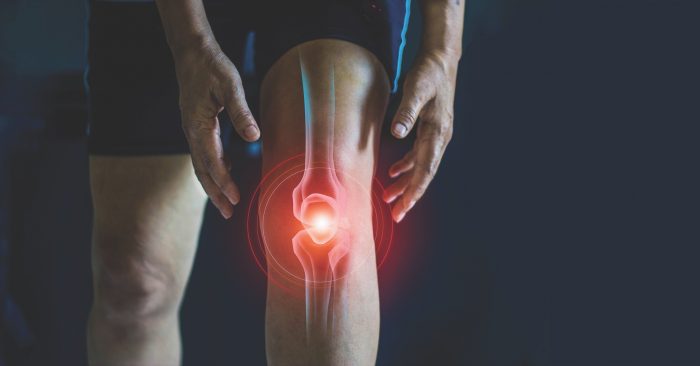
How long should you suffer with osteoarthritis?
The prevailing thought with osteoarthritis is that it is best to live with hip or knee pain as long as possible before having surgery. But when do we cross the line and potentially need joint replacement? In a study, those with osteoarthritis of the hip or knee joints that caused difficulty walking on a flat surface were at substantially greater risk of cardiovascular events, including heart attack (4). Those who had surgery for the affected joint saw a substantially reduced heart attack risk. If you have osteoarthritis, it is important to improve mobility, whether with surgery or other treatments. Of course, I have written in previous columns about techniques for managing osteoarthritis.
When does fiber matter most?
Studies show that fiber decreases the risks of heart attack and of death after a heart attack. In a recent analysis using data from the Nurses’ Health Study and the Health Professional Follow-up Study, results showed that higher fiber plays an important role in reducing the risk of death after a heart attack (5).
Those who consumed the most fiber, compared to the least, had a 25 percent reduction in post-heart attack mortality. Even more impressive is that those who increased their fiber after a cardiovascular event had a 31 percent reduction in mortality risk. The most intriguing part of the study was the dose response. For every 10-gram increase in fiber consumption, there was a 15 percent reduction in the risk of post-heart attack mortality. For perspective, 10 grams of fiber is a little over one cup of raspberries or two-thirds of a cup of black beans or lentils.
How much does lifestyle really affect heart disease risk?
In the Nurses’ Health Study, which followed 120,000 women for 20 years, those who routinely exercised, ate a quality diet, did not smoke and were a healthy weight demonstrated a whopping 84 percent reduction in the risk of cardiovascular events such as heart attacks (6).
We can substantially reduce the risk of heart attacks and even potentially the risk of death after sustaining a heart attack with modifications that include weight loss, physical activity and diet. While there are many diseases that contribute to heart attack risk, most of them are modifiable.
References:
(1) cdc.gov. (2) JAMA Intern Med. 2014;174(1):15-22. (3) Br J Sports Med. 2014, May 8. (4) PLoS ONE. 2014, 9: e91286 (5) BMJ. 2014;348:g2659. (6) N Engl J Med. 2000;343(1):16.
Dr. David Dunaief is a speaker, author and local lifestyle medicine physician focusing on the integration of medicine, nutrition, fitness and stress management. For further information, visit www.medicalcompassmd.com or consult your personal physician.