A new bill sponsored by Suffolk County Legislator Kara Hahn (D-Setauket) has been approved by the county Legislature.
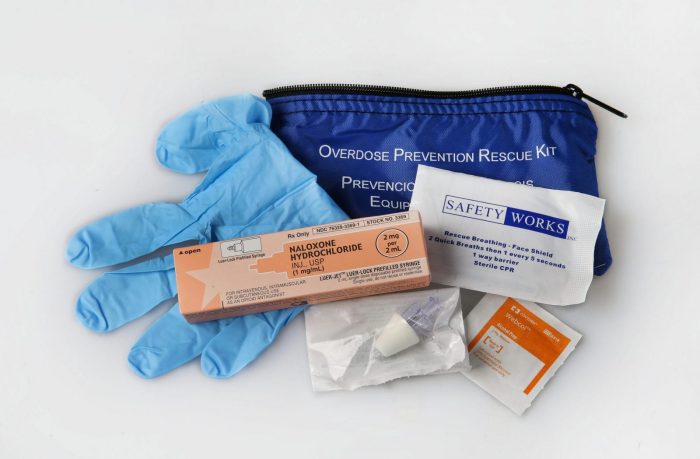
Her resolution requires kits of naloxone — or Narcan, its brand name — to be supplied in close proximity to automated external defibrillators in all county facilities. The bill was co-sponsored by county Legislator Tom Donnelly (D-Deer Park).
An April 4 press release stated that Narcan “is a lifesaving medication that can reverse the effects of an opioid overdose when administered in a timely manner.” Hahn believes this bill will help to improve the outcomes of the opioid overdoses seen in the county.
Hahn has been passionate about fighting the opioid epidemic for more than a decade now. In April of 2012, she sponsored a resolution which enabled police officers to administer Narcan to overdose victims. The press release for the current resolution noted, “According to SCPD statistics, patrol officers equipped with Narcan have saved thousands of lives in the 10 years since the [original] bill was enacted.”
Old Field resident Carole Trottere came up with the idea for this legislation and brought it to Hahn’s attention only a few months ago.
“It’s really a no-brainer,” Trottere said. “Put them in wherever we have AEDs. … If you save one life, it’s sparing the parents the horrible grief that I go through and giving someone a second chance to try to get into recovery.”
Trottere has been reaching out to grieving parent groups. “You cannot believe how many groups there are on Long Island alone and nationally of grieving parents who have lost children to fentanyl and overdoses,” she said.
She has also been working with the Suffolk County Police Department’s Behavioral Health Unit. Trottere lost her son, Alex Sutton, to a drug overdose in 2018, and last year planned an event in memory of him at his favorite pizza place. Police attended and carried out Narcan training at the event. This is something they would offer to anyone else who would like to plan an event in memory of a loved one.
According to the press release, the Long Island Council on Alcoholism and Drug Dependence also supports Hahn’s efforts.
She said this bill will be beneficial because Narcan kits need to be readily available. “What is frightening about the disease of addiction is that it can happen to anyone,” she added. “So it does need to be everywhere.”
Hahn also mentioned that street drugs are now sometimes laced with fentanyl, so someone could be taking what they think is a simple Xanax, but it’s actually unexpectedly laced with fentanyl.
“It’s probably the person who unexpectedly overdoses that will benefit the most from its placement,” she said. “If it’s ubiquitously placed, then more people will be saved.”
Hahn said she’s working with local universities to build the pipeline of clinical social workers, psychologists and psychiatrists that can help people battling mental health issues. She indicated the system is under-resourced, and she would like to work toward strengthening child, adolescent, and adult mental health in our communities.