With COVID-19 pandemic restrictions in the rearview mirror, residents have been returning to the open road and the open skies, visiting places and people.
In addition to packing sunscreen, bathing suits and cameras, local doctors urge people to check the vaccination status for themselves and their children, which may have lapsed.
“During COVID, many people did not keep up with their vaccines,” said Dr. Sharon Nachman, chief of the Division of Pediatric Infectious Diseases at Stony Brook Children’s Hospital. “That has led to a decrease in the amount of children who are vaccinated.”
Last week, the Centers for Disease Control and Prevention issued a health advisory to remind doctors and public health officials for international travelers to be on the lookout for cases of measles, with cases rising in the country and world.
As of June 8, the CDC has learned of 16 confirmed cases of measles across 11 jurisdictions, with 14 cases arising from international travel.
Measles, which is highly contagious and can range from relatively mild symptoms to deadly infections, can arise in developed and developing nations.
Measles can be aerosolized about 60 feet away, which means that “you could be at a train station and someone two tracks over who is coughing and sneezing” can infect people if they are not protected.
The combination of increasing travel, decreasing vaccinations and climbing levels of measles in the background creates the “perfect mixture” for a potential spread of the disease, Nachman said.
Typical first symptoms include cough, runny nose and conjunctivitis.
Conjunctivitis, which includes red, watery eyes, can be a symptom of numerous other infections.
“Many other illnesses give you red eyes,” Nachman said, adding, “Only when you start seeing a rash” do doctors typically confirm that it’s measles.
People are contagious for measles when they start to show these symptoms. Doctors, meanwhile, typically treat measles with Vitamin A, which can help ease the symptoms but is not an effective antiviral treatment.
As with illnesses like COVID, people with underlying medical conditions are at higher risk of developing more severe symptoms. Those with diabetes, hypertension, have organ transplants or have received anticancer drugs or therapies can have more problematic symptoms from measles.
In about one in 1,000 cases, measles can cause subacute sclerosing panencephalitis, or SSPE. About six to 10 years after contracting the virus, people can develop SSPE, which can lead to coma and death.
In addition to children who need two doses of the measles vaccine, which typically is part of the measles, mumps and rubella vaccine, or MMR, doctors urge people born between 1957 and 1985 to check on their vaccination status. People born during those years typically received one dose of the vaccine. Two doses provide greater protection.
Two doses of the MMR vaccine provide 97% protection from measles. One dose offers 93% immunity, explained Dr. David Galinkin, infectious disease specialist at Port Jefferson-based St. Charles Hospital.
People born before 1957 likely had some exposure to measles, which can provide lifelong immunological protection.
Nachman also urged people to speak with their doctor about their vaccination status for measles and other potential illnesses before traveling. People are protected against measles about two weeks after they receive their vaccine.
Doctors suggested that the MMR vaccine typically causes only mild reactions, if any.
Tetanus, Lyme
In addition to MMR vaccines, doctors urged residents to check on their tetanus vaccination, which protects for 10 years.
“The last thing you want to do is look for a tetanus vaccination in an international emergency room,” Nachman added.
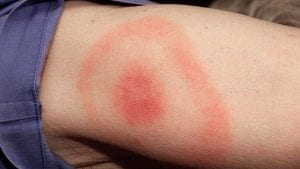
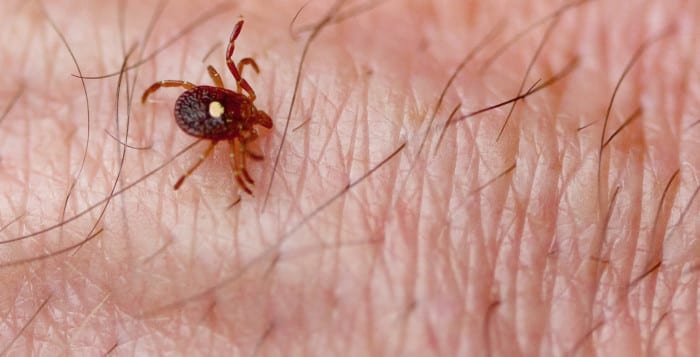
During the summer months, doctors also urged people to check themselves and their children, especially if they are playing outside in the grass or near bushes, for ticks.
Intermediate hosts for Lyme disease, a tick typically takes between 36 to 48 hours from the time it attaches to a human host to transmit Lyme disease.
Nachman suggested parents use a phone flashlight to search for these unwelcome parasites.